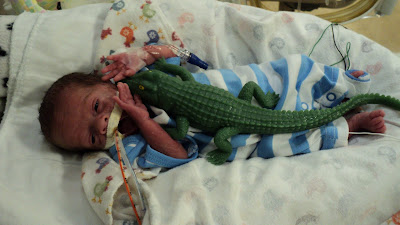
Mac turned one month old on Wednesday. Thirty days old and thirty weeks gestation. Yesterday, when we went to see him, there was a noticeable difference in his size. Because we see him everyday, it is hard to notice sometimes, but every once in a while we catch it and are amazed by how he has changed. He's bigger and stronger. Linda the amazing nurse tells us it is from wrestling crocodiles and fighting bears at night.
When he was born, he had almost no fat (so he had no butt cheeks...it was hilarious) and his skin was so papery thin, he was brick red because his blood was so visible. His head was still very mushy, and his eyes were fused. He looked like an adorable little alien baby.
Jon's ring fit on his perfect little foot.
I had never seen such a small baby. But then, I spent every day with him, and suddenly, I didn't see the tubes and wires anymore and instead of him looking small, all other babies started to look obscenely large.
Slowly, his eyes opened and he started looking more human. His skin got flaky, and then came back much thicker and, well, skin like. He has always had as much hair as Fabio though, good grief; look at that mop.
In the last week, though, he looks downright babyish to me. His cheeks are filling out (both sets!), he looks longer in the isolette, and he is more often alert and interacts more. It really is remarkable how much he has changed in just 30 days.
The last week was eventful. I already talked about his switch to the conventional ventilator, and he has done remarkably well on that. After a week though, they were still unable to get his vent settings weaned down and he was still producing a ton of secretions, so his lungs continued to be really cloudy, and are starting to become scarred as a result of the inflammation, so we started discussing the use of dexamethasone again. The difference was, this time the idea was to use it to extubate, as opposed to using it as a treatment for Chronic Lung Disease. I had also had several discussions with other doctors about how it is used here and the differences in protocol between here and the studies I had read, and was feeling more comfortable with it's use. They use smaller doses and start when the babies are older, which decreases the risk of developmental disorders. They started it on Friday and he has done really well on it. His vent settings have come consistently down. We're hoping that we can switch him to the CPAP (like what people who have sleep apnea wear) on Friday and get rid of that tube so his lungs can start to heal, and so I can see his cute mouth. This is a pretty big step and we are pretty excited, so keep fingers crossed that he responds well.
The other thing that happened this last week is that he decided he had had enough of his tube and extubated himself.
Ok, so that isn't quite what happened. What actually happened is that he got some fluid in his tube while I was holding him as a result of some medicine they had given to thin the secretions. He waterboarded himself and, in the process of freaking out (who wouldn't), he did a pushup with his super micropreemie strength and pulled the tube out of his wind pipe. This led to several minutes of bluish grey skin, resuscitation, and panic among family members (mom and me) and determined amazingness among the respiratory therapist and nurse (go Pam and Val!).
Makes you realize (again) how fragile this life is, not just for these little ones, but for all of us. So, we revel in the beauty around us, love as much as we can, forgive, enjoy the time we've been given, and eat dessert first.
Oh, and express gratitude. I hope you all know how aware of and grateful we are for your prayers and love and support. We couldn't ask for better friends and family. Or strangers, for that matter...we know you're out there lurking and following our story through mutual friends. I hope our story brings you hope and you can share our joy. That is part of what this life is about, after all.
The Newbury Girls aren't afraid to try new things, thirst and hunger for knowledge, and have great joy in participating in this most uncivilized adventure called life.

Tuesday, June 28, 2011
Monday, June 20, 2011
Mother's and Father's Day
We've dubbed this the best year for parent's day ever. For more than the obvious reasons.
I'll explain.
Thursday, our update was not so happy. McKell's lungs were still super hazy, he was still very full of secretions, they are feeling pretty confident that he is developing a nice case of chronic lung disease, and so they just couldn't seem to get the vent settings down without his O2 plummeting. We couldn't even look at him wrong without it dropping. During his diaper change one night, his sats were in the 60s (they should be between 84 and 94) and his supplemental oxygen was at 100%. He was needing between 50% and 60% supplemental oxygen just to keep his head above water at the best of times. The air we breathe is about 21%.
The doc who rounded on him that day (there are about 15 at this hospital) warned me we were probably going to have to use a steroid called dexamethasone to wean him down and reduce the inflammation. I had read a couple of studies that indicated it had some potential long term developmental implications, and I was concerned about using it before we tried other options. I was assured that our other options were limited though, and that if we switched him to a conventional ventilator, he was likely to lose lung volume and have to be put back on the other vent. I pushed just a little bit. I prayed even more...something along the lines of, "I don't like the idea of this drug. Bless the docs that they can find another way. If not, protect his brain." Sometime while all of this was happening, someone "accidentally" changed one of the vent settings. No one knows who or why. I don't understand the details, but for some reason, because of how well his lungs responded to that, Friday morning they decided to give the conventional vent a try before they did anything else. One of respiratory therapists assured me he would fail. And then they all waited for his O2 sats to plummet.
And they waited.
And he breathed. And his lungs stayed the same (which was acceptable; at least they didn't get worse). He was pretty agitated and was a little swingy in his O2 needs, but not worse. They told me that once calmed down and stabilized, in a day or two, I would be able to hold him.
I plotted. I bided my time. I counted my victories for the day against the day shift (I say that a bit tongue in cheek. They were not at all resentful or obnoxious about throwing out many years of medical experience and intuition and listening instead to some psycho who had spent a couple of hours on the internet. Who needs medical school?) I knew who was on night shift. I thought I might be able to convince them that he just needed his mama.
I was not disappointed. The team on night shift thought it was a great idea and laid him on my chest. His oxygen saturation had been in the low 80s with 45-50% supplemental oxygen. His heart rate had been about 180. It took about three minutes, and his O2 saturation skyrocketed (this is good). They turned his FIO2 (supplemental oxygen) down. Then they turned it down again. Then again. In about ten minutes, his FIO2 was at 26% and his saturation was at about 92. His heart rate was about 160. His breathing was stable and steady. We both breathed a collective sigh. It was awesome. I held him for about an hour an a half. When we had to go home, they put him in his isolette (incubator), changed his diaper, retaped his breathing tube, and reswaddled him, and never once did he need more than 30% O2. He stayed stable through the night, slept great, and the next morning, his lungs looked better. We are now on day 3 on this vent, holding him twice a day, and he is much improved (we all are). They were even able to wean his vent settings a bit.
There is definitely something healing about human touch. I feel healed already.
I'll explain.
Thursday, our update was not so happy. McKell's lungs were still super hazy, he was still very full of secretions, they are feeling pretty confident that he is developing a nice case of chronic lung disease, and so they just couldn't seem to get the vent settings down without his O2 plummeting. We couldn't even look at him wrong without it dropping. During his diaper change one night, his sats were in the 60s (they should be between 84 and 94) and his supplemental oxygen was at 100%. He was needing between 50% and 60% supplemental oxygen just to keep his head above water at the best of times. The air we breathe is about 21%.
The doc who rounded on him that day (there are about 15 at this hospital) warned me we were probably going to have to use a steroid called dexamethasone to wean him down and reduce the inflammation. I had read a couple of studies that indicated it had some potential long term developmental implications, and I was concerned about using it before we tried other options. I was assured that our other options were limited though, and that if we switched him to a conventional ventilator, he was likely to lose lung volume and have to be put back on the other vent. I pushed just a little bit. I prayed even more...something along the lines of, "I don't like the idea of this drug. Bless the docs that they can find another way. If not, protect his brain." Sometime while all of this was happening, someone "accidentally" changed one of the vent settings. No one knows who or why. I don't understand the details, but for some reason, because of how well his lungs responded to that, Friday morning they decided to give the conventional vent a try before they did anything else. One of respiratory therapists assured me he would fail. And then they all waited for his O2 sats to plummet.
And they waited.
And he breathed. And his lungs stayed the same (which was acceptable; at least they didn't get worse). He was pretty agitated and was a little swingy in his O2 needs, but not worse. They told me that once calmed down and stabilized, in a day or two, I would be able to hold him.
I plotted. I bided my time. I counted my victories for the day against the day shift (I say that a bit tongue in cheek. They were not at all resentful or obnoxious about throwing out many years of medical experience and intuition and listening instead to some psycho who had spent a couple of hours on the internet. Who needs medical school?) I knew who was on night shift. I thought I might be able to convince them that he just needed his mama.
I was not disappointed. The team on night shift thought it was a great idea and laid him on my chest. His oxygen saturation had been in the low 80s with 45-50% supplemental oxygen. His heart rate had been about 180. It took about three minutes, and his O2 saturation skyrocketed (this is good). They turned his FIO2 (supplemental oxygen) down. Then they turned it down again. Then again. In about ten minutes, his FIO2 was at 26% and his saturation was at about 92. His heart rate was about 160. His breathing was stable and steady. We both breathed a collective sigh. It was awesome. I held him for about an hour an a half. When we had to go home, they put him in his isolette (incubator), changed his diaper, retaped his breathing tube, and reswaddled him, and never once did he need more than 30% O2. He stayed stable through the night, slept great, and the next morning, his lungs looked better. We are now on day 3 on this vent, holding him twice a day, and he is much improved (we all are). They were even able to wean his vent settings a bit.
There is definitely something healing about human touch. I feel healed already.
Labels:
Mac
Tuesday, June 14, 2011
Day 20
The last week has gone by really fast. The last three weeks have actually been quite a blur, to be honest. But something in the doctors' tones has recently changed. Instead of focusing on the next day, or even hour, they are talking in terms of weeks and even months. They are generally more optimistic, even though McKell's little lungs are still struggling to catch up with him. He's on what they call full feedings, meaning he is getting all of his calories by mouth instead of by IV. They are trying to wean him off of he ventilator he is on and move him to a conventional vent, which would mean I could hold him, and it would do less damage to his lungs. But they are getting progressively better...even though we feel like we take a step back for every two steps forward. It is a long road, and we are not out of the woods yet, but we can see the light up ahead.
Labels:
Mac
Saturday, June 11, 2011
Two Pounds!
Last night, McKell hit the two pound mark. They also had to turn his bed temperature down because he is maintaining his heat better. Yay for growth!
Otherwise, not much has changed (hence the lack of updates the last two days). His lungs are still pretty crappy, but as I understand it, it is a question of just maintaining a holding pattern until he gets bigger (which he's doing: TWO POUNDS!) and his lungs mature. The problem is, how much damage is done to the lungs in the mean time? Who knows? No one. So we still take it one day at a time.
He is still eating reasonably well. He is up to ten ml every three hours, and is digesting it pretty well. And he's getting about 40% of his calories from me, as opposed to the IV. It is amazing the things you worry about with preemies. Sheesh.
And just so you know, I don't have man hands. I have normal sized hands. He is just ridiculously small. But fat...two pounds. My goodness.
Otherwise, not much has changed (hence the lack of updates the last two days). His lungs are still pretty crappy, but as I understand it, it is a question of just maintaining a holding pattern until he gets bigger (which he's doing: TWO POUNDS!) and his lungs mature. The problem is, how much damage is done to the lungs in the mean time? Who knows? No one. So we still take it one day at a time.
He is still eating reasonably well. He is up to ten ml every three hours, and is digesting it pretty well. And he's getting about 40% of his calories from me, as opposed to the IV. It is amazing the things you worry about with preemies. Sheesh.
And just so you know, I don't have man hands. I have normal sized hands. He is just ridiculously small. But fat...two pounds. My goodness.
Labels:
Mac
Wednesday, June 8, 2011
Two Weeks Old
Day 14. Two weeks old. It was a quiet day. His O2 was mostly stable. Both eyes are open. He's getting 5ml of food every three hours, which now accounts for about 40% of his total calories (it was about 11% a week ago). His blood looks good. His arterial line went in without a hitch.
But,
His hemoglobin is down, so he needs another transfusion, which means another IV line. His blood pressure is questionable, so there is a slight chance that his arterial duct is open again. The arterial line is in his wrist and so his whole arm is braced. And his lungs are still crappy looking.
So, we wait and hope and pray and thank our stars so many people are doing the same.
But,
His hemoglobin is down, so he needs another transfusion, which means another IV line. His blood pressure is questionable, so there is a slight chance that his arterial duct is open again. The arterial line is in his wrist and so his whole arm is braced. And his lungs are still crappy looking.
So, we wait and hope and pray and thank our stars so many people are doing the same.
Labels:
Mac
Tuesday, June 7, 2011
Lucky 13
Well, today Mac lost the line into the artery in his umbilical cord, so he will get a new 'ART' line today, either in his wrist or ankle. He still isn't showing signs of infection, but his lungs are still not healthy. He can't see to regulate his oxygen and the ventilator is causing his lungs to be full of gunk. So, we're working on that. Otherwise, he is taking milk (through a tube, but we take what we can get), and he's gaining weight. He'll be two pounds in NO time.
Labels:
Mac
Monday, June 6, 2011
Day 12 of a most uncivilized adventure...
He is 12 days old today. It's amazing, considering I feel like I've been here a year. I know all the bells and alarms, know all about PIE, PDA, and brain bleeds, and have developed a nice friendly relationship with all of the nurses. I think God just wants me to be 100% sure I REALLY want this little guy (I do). Right now, he is stable. He is tolerating his feedings well, which is nice considering I hook my bosom up to what looks like a cold war era torture device six times a day and twice in the middle of the night. He has no bleeding in the brain, his heart valve is closed, and his blood gasses look great. His lungs are causing us some grief, but considering he was counting on three more months to develop them, you can't really blame him. All in all, we are still optimistic, and are happy to have such great care here at Utah Valley. I'll start posting the daily updates we receive here, so if you are interested, you can check in here for the roller coaster ride.
Labels:
Mac
Subscribe to:
Posts (Atom)